
February 13, 2026
A Healthy Ramadan Nourished Body and Mind
It's that beautiful time of year again with the start of Ramadan just around the...
December 26, 2024
Rediscovering the Forgotten Fifth Class of G Proteins
G proteins are essential molecular switches in the body, responsible for transmi...

November 11, 2024
Safety Management and Individual Safety Performance
Safety Management (SM) and Individual Safety Performance (ISP) are essential to ...
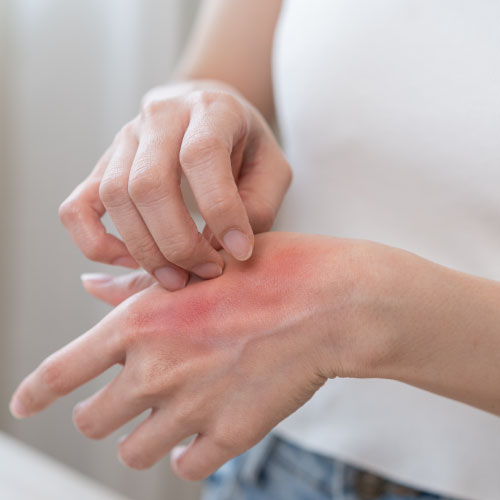
Atopic dermatitis (AD) is a common, chronic skin condition that many, especially...

October 23, 2024
Sleep your Way to a Slimmer Waist
It's late, and you know you should get to bed. But maybe there's just one more e...

July 23, 2024
What is Climate Finance?
As the world reflects on the outcomes of COP28, "climate finance" has emerged as...

July 22, 2024
Understanding blockchain and cryptocurrency in 2024
The words 'blockchain' and 'cryptocurrency' are now firmly established into our ...

When it comes to carbon emissions, the aviation industry is one of the worst cul...

This February, Australia became the latest country to officially pass 'right to ...
